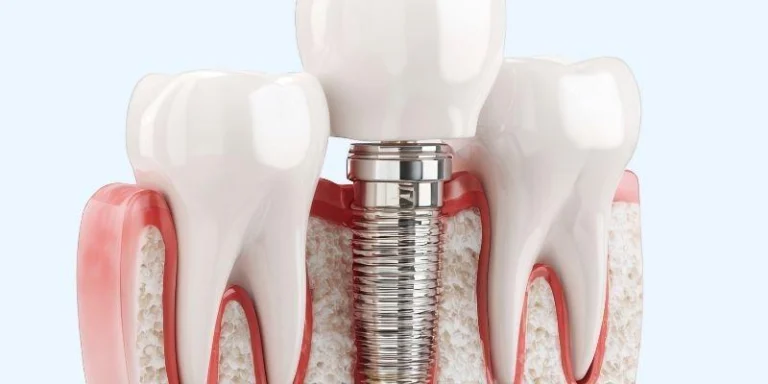
Most people think the surgery is the hardest part of getting dental implants. But the truth is that what happens before you sit in the surgical chair matters much more, highlighting the dental implant planning importance.
The planning phase determines where your implant goes, how it fits with your bone and anatomy, and whether it will last for decades or cause problems down the road.
When dentists use digital planning and 3D imaging to guide implant placement, they can see exactly where nerves and sinuses are located. They can measure your bone density and plan the perfect angle before making a single cut. This level of detail helps avoid complications and sets you up for long-term success.
Think of it this way: surgery is just following the plan. If the plan is rushed or incomplete, even perfect surgical technique cannot fix poor positioning. That’s why understanding how your implant is planned gives you better control over your treatment outcome.
Key Takeaways
- Dental implant planning uses 3D imaging and digital tools to determine exact implant position before surgery begins
- Proper planning evaluates your bone structure, nearby nerves, and bite forces to reduce complications and improve long-term results
- The surgery itself follows the plan, so careful preparation matters more than the procedure for lasting implant success
Why Proper Dental Implant Planning Is Crucial
The planning phase determines whether your dental implants will function properly for decades or lead to complications that require additional procedures. Poor planning increases your risk of implant failure, nerve damage, and aesthetic problems that affect your smile and bite.
Impact on Long-Term Implant Success
Careful planning helps avoid problems and ensures your implants last as long as possible. Your dentist needs to evaluate your bone density, gum health, and bite alignment before surgery. These factors directly affect how well your implant integrates with your jawbone.
Studies show that implants placed with detailed planning have higher success rates than those placed without proper evaluation. Your dentist must consider where nerves and blood vessels are located to avoid damaging them during surgery.
The planning phase also identifies any existing health issues that could interfere with healing. If you have gum disease or insufficient bone, these problems need treatment before implant placement. Addressing these concerns early prevents complications that could cause your implant to fail years later.
Risks of Inadequate Planning
Skipping thorough planning can lead to serious problems during and after your procedure. Implants placed in the wrong position may not support your replacement teeth properly. This creates bite problems and can damage the implant over time.
Without proper imaging, your surgeon might place an implant too close to a nerve. This can cause pain, numbness, or tingling that lasts for months or becomes permanent. Common challenges in dental implant planning include inadequate bone assessment and failure to account for anatomical structures.
Poor implant positioning also creates aesthetic issues. If an implant sits too far forward or at the wrong angle, your crown won’t look natural. You might also experience implant failure if the bone cannot support the implant because of insufficient planning.
Comparing Guided and Freehand Placement
Guided surgery methods help lower complication risks and speed up recovery compared to freehand techniques. Guided implant surgery uses 3D imaging and surgical guides that show your dentist exactly where to place your implant.
Key differences between approaches:
| Guided Placement | Freehand Placement |
| Uses 3D scans and surgical templates | Relies on dentist’s visual assessment |
| More precise implant positioning | Higher margin of error |
| Shorter surgery time | Longer procedure |
| Better outcomes for complex cases | May work for simple cases |
With guided implant surgery, your dentist creates a custom template based on digital scans of your jaw. This template fits over your gums during surgery and directs the drill to the exact position planned on the computer. The result is more accurate implant placement that reduces trauma to surrounding tissue.
Core Steps in the Dental Implant Planning Process
Getting dental implants involves careful preparation that happens before any surgery takes place. Your dentist follows specific steps to evaluate your mouth, capture detailed images, and design a plan that fits your unique needs.

Comprehensive Oral and Medical Evaluation
Your dental implant consultation starts with a thorough dental exam where your dentist reviews your complete medical history. This helps identify any health conditions that might affect implant success, such as diabetes or heart disease.
During the comprehensive evaluation, your dentist checks your gum health, bone density, and any existing dental work. They look for signs of gum disease or infections that need treatment first. You’ll discuss medications you take since some can affect healing.
Your dentist also asks about your goals and expectations. This conversation helps them understand what you want from your new teeth. They’ll explain what’s realistic based on your specific situation.
Diagnostic Imaging and Assessment
Advanced imaging techniques give your dentist a complete view of your jaw structure. Standard dental X-rays provide basic information, but CBCT scans offer much more detail.
Cone beam CT creates three-dimensional images of your jawbone, nerves, and sinuses. This 3D imaging shows exactly how much bone you have and where important structures sit. Your dentist uses cone-beam computed tomography to measure bone quality and identify the safest spots for implant placement.
Digital planning software lets your dentist map out the exact angle and depth for each implant. This diagnostic imaging helps avoid nerves and ensures implants support your new teeth properly.
Creating a Personalized Treatment Plan
Your dentist combines all the information from your exam and scans to build your surgical plan. They decide how many implants you need and where to place them for the best results.
The personalized treatment plan includes the type of implants that work best for your bone structure. Your dentist considers how your final teeth will look and function. They create surgical guides based on your digital planning to ensure precise placement during surgery.
You’ll receive a timeline showing each phase of treatment. This includes any bone grafting needed, healing periods, and when you’ll get your permanent teeth.
Our specialists provide advanced implant planning across Fredericksburg, Fairfax, Manassas, and Stafford in VA. Book your personalized evaluation today.
Anatomical and Structural Considerations Before Surgery
Your jawbone structure, soft tissue health, and the location of vital nerves determine whether an implant can be placed safely and successfully. Understanding these factors before surgery helps prevent complications and ensures long-term stability.
Bone Quality, Volume, and Grafting Needs
Your bone density and bone volume are the foundation for any dental implant. The jawbone needs to be thick enough and strong enough to support the implant fixture. If you’ve experienced bone loss due to missing teeth, periodontal disease, or trauma, your bone structure may not be adequate for immediate placement.
Bone grafting becomes necessary when your natural bone can’t support an implant on its own. Your dentist evaluates the width and height of available bone to determine if you need augmentation. Class I defects involve reduced width, Class II involves reduced height, and Class III involves both dimensions.
Common situations requiring bone grafts:
- Tooth loss that occurred months or years ago
- Previous infections or gum disease
- Natural bone resorption after extraction
- Insufficient bone near the maxillary sinus
The quality of your bone matters as much as the quantity. Dense bone provides better stability than softer bone. Your treatment team assesses these factors through imaging to plan the right approach for your specific anatomy.
Gum and Soft Tissue Health
Your gum health directly impacts implant success rates. If you have active periodontal disease, placing an implant without treating the infection first increases your risk of peri-implantitis. This condition causes inflammation around the implant and can lead to failure.
Healthy gums provide a protective seal around the implant. They prevent bacteria from reaching the bone and help maintain stability over time. Your dentist examines your soft tissues for signs of infection, inflammation, or inadequate thickness before moving forward.
Thin or damaged gum tissue may need grafting to create proper coverage. The tissue around your implant site must be thick enough to support healing and provide long-term protection. Poor gum health delays treatment until these issues are resolved.
Protecting Nerves, Sinuses, and Neighboring Structures
Critical anatomical structures must remain undamaged during implant placement. The inferior alveolar nerve runs through your lower jaw and provides sensation to your lip and chin. Damaging this nerve causes numbness or pain that may be permanent.
Your implant needs to stay at least 2.5-3 mm away from nerves and sinuses. In your upper jaw, the maxillary sinus sits above the back teeth. If you don’t have enough bone height, your dentist may recommend a sinus lift to create adequate space without penetrating the sinus cavity.
Safety distances for implant placement:
| Structure | Minimum Distance |
| Inferior alveolar nerve | 2.5-3 mm |
| Mental foramen | 4 mm |
| Adjacent teeth | 1.5 mm |
| Between implants | 3 mm |
The mental foramen, where nerves exit your jawbone, requires special attention. Planning must account for an anterior loop that extends forward from this opening. Blood vessels near the lingual plates also need protection during surgery to prevent bleeding complications.
Prosthetically Driven Planning and Implant Positioning
Prosthetically driven implant planning means starting with your final restoration in mind before placing any implant. The position, angle, and depth of your implant determine how well your replacement tooth functions and looks in your mouth.
Restoration and Bite Alignment Goals
Your prosthodontist needs to plan backward from the tooth you want. This means designing the crown or bridge first, then figuring out where the implant should go to support it properly.
When your dentist uses this approach, they can make sure your new tooth lines up correctly with your bite. Poor bite alignment causes problems like chewing difficulty, jaw pain, and uneven wear on your other teeth.
The abutment that connects your implant to the crown needs the right amount of space and correct angulation. If your implant sits too far forward, backward, or at the wrong angle, your prosthodontist might not be able to create a natural-looking restoration.
Digital planning tools let your dental team visualize these relationships before surgery happens.
Angulation, Depth, and Position Accuracy
Your implant position affects everything about your tooth replacement. The implant needs to sit at the right depth in your jawbone so the crown emerges naturally from your gum tissue.
Key positioning factors include:
- Angulation: Tilted implants can make it hard to attach straight crowns
- Depth: Too shallow or too deep affects implant stability and appearance
- Horizontal placement: Side-to-side position impacts gum contours and cleaning access
Even small positioning errors of 1-2 millimeters can create big problems. Your implant might end up too close to nearby teeth or nerves. The bone quality at the planned site matters too, since implant stability depends on solid bone contact during healing.
Ready for implants? Visit our clinic, Greater Washington Oral & Maxillofacial Surgery, to start your digitally guided treatment plan.
Challenges and Solutions in Implant Planning
Even with advanced technology, dental professionals face real obstacles when creating implant plans. Insufficient bone density, patient health conditions, and unrealistic expectations can all derail treatment before the oral surgery even begins.
Addressing Complex Cases and Anatomical Limitations
Your jawbone structure plays a critical role in dental implant treatment success. When you don’t have enough bone density or volume, your periodontist needs to plan for bone grafting procedures before placing implants.
Anatomical challenges require careful navigation. Your sinus cavities, nerve pathways, and existing tooth roots all create boundaries that oral surgeons must work around. Advanced imaging techniques like CBCT scans provide three-dimensional views that help identify these obstacles early.
Some patients present with complex medical histories or unusual jaw anatomy. Your dental team might need to collaborate with specialists to develop modified approaches. Digital planning tools allow professionals to simulate different placement angles and positions before touching your mouth.
Overcoming Patient Health and Lifestyle Barriers
Your overall health directly impacts implant success rates. Conditions like uncontrolled diabetes, osteoporosis, or autoimmune disorders require special consideration during the planning phase.
Smoking presents one of the biggest challenges in implant prosthodontics. If you smoke, your dentist will likely recommend quitting several weeks before dental implant surgery to improve healing outcomes.
Certain medications can interfere with bone healing and osseointegration. Your oral surgeon needs to review all prescriptions and supplements you take. Sometimes adjusting medication timing or working with your physician to find alternatives becomes necessary.
Same-day implants aren’t appropriate for everyone. Your bone quality and health status determine whether immediate placement is safe or if you need a staged approach.
Setting Realistic Expectations
You might want quick results, but rushing the process often leads to failure. Your periodontist should explain that proper healing between stages takes months, not weeks.
Not everyone qualifies as a candidate for implant surgery right away. You may need preparatory procedures that extend your treatment timeline. Understanding these requirements upfront prevents disappointment later.
Your final results depend heavily on factors beyond the surgical procedure itself. Proper planning accounts for how your bite works, your facial structure, and your aesthetic goals to create functional and natural-looking teeth.
From Surgical Guide to Procedure: How Planning Shines in Surgery
The surgical guide transforms your digital plan into physical reality during the procedure, ensuring precise implant placement while reducing surgery time and post-operative discomfort.

Role of Custom Surgical Guides
Custom surgical guides translate your virtual implant plan into a physical template that directs drill positioning during surgery. These guides fit over your teeth, gums, or bone to control where the implant goes.
Your dentist chooses from three types based on your situation. Tooth-supported guides rest on your remaining teeth and offer the best stability. Mucosa-supported guides sit on your gums when you’re missing all teeth in an area. Bone-supported guides attach directly to the bone after your dentist makes a small opening.
The guide contains metal sleeves that direct the drill at the exact angle and depth planned on the computer. These sleeves have specific measurements—typically 2.0-5.0mm inner diameter and 5-10mm height—that match your implant system. Your dentist positions the guide once, and it stays stable throughout the entire procedure without constant adjustments.
Benefits to Patient Experience and Recovery

Guided implant surgery simplifies the placement process and reduces your time in the dental chair by up to 50% for complex cases. You experience less discomfort because your dentist makes smaller, more precise movements.
Many procedures using guides don’t require cutting and lifting your gums. This flapless approach means you heal faster with less swelling and pain. You can often return to normal activities within a day or two instead of waiting a week.
The timing of implant placement becomes more predictable with guided surgery. Your dentist can confidently schedule immediate implant placement right after tooth extraction because the guide ensures proper positioning. You might even receive a temporary tooth the same day, walking out with a complete smile rather than a gap.
How Planning Reduces Complications
Planning for dental implants through surgical guides helps reduce complications by maintaining safe distances from nerves and sinuses. The guide keeps your implant at least 2mm away from the nerve in your lower jaw and 1mm from your sinus floor.
Your implant stays properly positioned relative to neighboring teeth—maintaining 1.5mm clearance from natural teeth and 3mm between multiple implants. This spacing protects your bone and prevents long-term problems. Studies show guided surgery has a 2-5% complication rate compared to 5-15% with freehand placement.
The guide also prevents your dentist from placing the implant too deep or too shallow. Your final crown will emerge naturally from your gums rather than looking awkward or artificial.
Take the first step toward a confident smile. Schedule your implant consultation today to see how precise planning sets the foundation for long-term success.
Frequently Asked Questions
Proper planning affects everything from how well your implant integrates with your jawbone to whether you’ll need extra procedures like bone grafts. The consultation phase determines candidacy, reduces risks, and sets realistic expectations for your new smile.
How does thorough planning impact the success of dental implant procedures?
Detailed planning creates a roadmap for your entire treatment. Your dentist examines your bone density, gum health, and bite alignment to determine the exact placement for each implant.
When you skip proper planning, implants may be placed at the wrong angle or depth. This can lead to implant failure or an uncomfortable bite. Studies show that careful planning during consultations leads to higher success rates because potential problems are identified before surgery begins.
Your dentist also uses planning to decide if you need additional procedures first. Some patients require bone grafts or treatment for gum disease before implants can be placed safely.
In what ways can pre-surgical planning minimize potential complications in dental implant surgeries?
Pre-surgical planning helps your dentist spot potential problems before they happen. During your consultation, imaging reveals the location of nerves, sinuses, and blood vessels that must be avoided during surgery.
Your medical history review identifies conditions that could affect healing. Uncontrolled diabetes, certain medications, and smoking habits all impact how well your body accepts the implant. When these issues are addressed beforehand, you have a much better chance of successful healing.
Planning also determines if your jawbone is strong enough to support implants. If your bone has weakened from tooth loss, your dentist can schedule a bone graft procedure first. This extra step may add time to your treatment, but it prevents implant failure later.
Why is understanding a patient’s oral anatomy crucial before proceeding with a dental implant?
Every mouth is different. Your jawbone thickness, nerve pathways, and sinus locations are unique to you.
Without understanding your specific anatomy, a dentist might accidentally damage nerves or place an implant where there isn’t enough bone support. 3D scans and X-rays taken during planning show the exact structure of your jaw. This information guides the surgeon to place implants safely and precisely.
Your bite pattern also affects implant placement. If your upper and lower teeth don’t meet properly, implants need to be positioned to match your natural bite. Otherwise, you might experience discomfort when chewing or speaking.
How does the quality of initial consultations affect the long-term success of dental implants?
A thorough initial consultation sets the foundation for implants that last decades. During this appointment, your dentist evaluates everything from your oral health to your lifestyle habits.
Your consultation includes a comprehensive planning session that assesses whether you’re a good candidate. Patients who receive detailed consultations understand what to expect during recovery and how to care for their implants afterward. This knowledge helps them follow aftercare instructions more carefully.
The quality of your consultation also affects how well your final restoration looks. When your dentist takes time to understand your aesthetic goals, they can design implants that match your natural teeth in color, shape, and size.
What advanced technologies are used in planning for dental implants and how do they benefit the patient?
Cone Beam CT scans create 3D images of your jaw that show bone quality and nerve locations. This technology gives your dentist a complete view of your mouth from every angle. Regular X-rays only show two dimensions, but 3D imaging reveals details that prevent complications.
Intraoral scanners take digital impressions of your teeth without messy molds. These scans are more accurate and comfortable than traditional methods. The digital files can be used to design your implants with computer software.
Computer-guided implant placement uses software to map exactly where each implant should go. The dentist creates a surgical guide based on your 3D scans. During surgery, this guide ensures implants are placed at the precise angle and depth planned beforehand.
Can you explain the role of a detailed treatment plan in achieving a natural look and feel with dental implants?
Your treatment plan determines how your final restoration will look in your mouth. During planning, your dentist considers your facial structure, gum line, and the color of your existing teeth.
The plan includes the size and shape of your implant crown. If the crown is too large or small, it won’t look natural next to your other teeth. Your dentist also plans for proper spacing so your implants don’t crowd neighboring teeth.
A detailed plan addresses your gum tissue, too. The implant needs to emerge from your gums at the right angle to match your natural teeth. When planning accounts for all these factors, your implants look and function just like the teeth you were born with.