Prevalence and National Trends: Wisdom tooth (third molar) extractions are extremely common in the U.S. – estimates suggest roughly 10 million wisdom teeth (about two per patient) are removed annually, affecting ~5 million Americans each year.
Insurance-claims data indicate that about half of privately insured young adults have had at least one wisdom tooth removed by age 25, rising to roughly 70% by age 60. Extractions are performed slightly more often in women than men (adjusted risk ~8% higher for females).
Many extracted teeth are impacted, but others are fully erupted; overall, about 37% of individuals globally have at least one impacted wisdom tooth. In practice, most extraction episodes involve removing multiple teeth (often all four).
Dentists commonly advocate removal of diseased or high-risk wisdom teeth, but opinions vary on asymptomatic teeth.
According to dental surveys, general dentists recommended removal (often prophylactically) in ~59% of adolescent cases, with retention and monitoring advised for the rest when wisdom teeth are clearly healthy and well-positioned.
Get expert wisdom teeth evaluations and removal care in Northern Virginia.
Age Distribution of Wisdom Tooth Management

Figure: Age distribution of wisdom tooth extraction procedures (adapted from a large multi-center study) – impacted wisdom teeth (blue curves) are removed mostly around age 18–20, whereas erupted extractions (orange curve) peak later.
Third molars typically emerge in the late teens to early 20s, and accordingly most extractions occur in that age range. A large analysis of patient records found that while the mean patient age at third-molar removal was ~31 years for women and ~35 years for men, the modal age was in the late teens (18–20 years old).
In other words, most extractions cluster around age 18–21. By the mid-20s, about half of patients have had at least one wisdom tooth removed; beyond that age extractions continue gradually, often for late-presenting pathologies. (Data from insurance claims imply ~50% incidence by age 25 and ~70% by age 60.)
Dentists’ decision-making reflects this age trend. In a prospective U.S. cohort of 16–22 year-olds, removal was recommended for many patients to “prevent future problems” (79% of extractions cited prophylactic reasons).
When dentists opted not to remove asymptomatic third molars, it was often because they planned to monitor them (“too early to decide” in 73% of those cases).
Clinical guidelines generally align with a watchful-waiting approach: a recent Cochrane review concluded that evidence is insufficient to justify routine removal of disease-free impacted wisdom teeth.
In practice, asymptomatic wisdom teeth are usually monitored via periodic exams (e.g. every 6–12 months) rather than automatically extracted.
Schedule a consultation to review your wisdom teeth risks and treatment options.
Extraction vs. Monitoring: Evidence and Guidelines
Removal of wisdom teeth is clearly indicated when disease is present (pericoronitis, cysts, caries, orthodontic needs, etc.), and most clinicians agree on extracting symptomatic wisdom teeth. The debate is over asymptomatic, pathology-free third molars.

In the U.S., guidelines and practice trends have shifted toward individual risk assessment.
The American Association of Oral and Maxillofacial Surgeons advises extracting third molars that pose a “high risk” of future disease, but many public health experts (including the American Public Health Association) caution against blanket prophylactic removal without clear indication.
Retaining a healthy wisdom tooth simply requires scheduling routine dental check-ups; if any pathology arises later (e.g. deep caries, recurrent pericoronitis), then extraction is pursued. In short, current practice involves a mix of early extraction (for obvious risk factors) and planned monitoring.
Data suggest that roughly half of wisdom teeth that are not initially removed will eventually be extracted before old age, while the rest remain intact or are removed later if needed.
Get a personalized plan based on your age, tooth position, and risk factors.
Complication Rates (U.S. Data)
All surgeries carry risk, and third-molar surgery is no exception. Fortunately, most complications are infrequent. Common adverse events include pain, swelling and trismus, which occur in the majority of cases but are generally self-limiting. More concerning complications have lower incidences:
- Dry Socket (Alveolitis): This delayed healing of the extraction socket occurs when the blood clot is lost. Reported rates vary, but recent large analyses place it around 3–4% of routine extractions (perhaps slightly higher for mandibular extractions in young adults).
- Postoperative Infection: Overall infection at the surgical site is uncommon. A meta-analysis estimated an overall surgical-site infection rate of only 1.7% (95% CI ~1.0–2.6%) following impacted third molar extraction. Prophylactic antibiotics are sometimes used, but standardized protocols vary.
- Inferior Alveolar Nerve Injury: This is the most feared complication. Temporary numbness of the lower lip/chin can occur in up to roughly 1–3% of wisdom tooth extractions, depending on impaction depth and surgeon experience. Permanent injury is rarer, usually under about 2% of cases. Most nerve injuries (especially in young patients) recover over weeks to months.
- Lingual Nerve Injury: This causes tongue numbness or altered taste. Recent systematic reviews report permanent lingual nerve damage in only about 0.04–0.6% of third-molar surgeries. Temporary lingual numbness (from flap retraction) is higher (up to ~10% in some series) but usually resolves within weeks.
Other complications (e.g. heavy bleeding, jaw fracture, TMJ dysfunction) are extremely rare. Thus, modern rates of serious complications are low, but given the high volume of procedures nationally, they still affect many patients (e.g. hundreds of thousands per year may experience a dry socket or transient nerve issues).
Regional Patterns in Virginia (Urban vs. Rural)
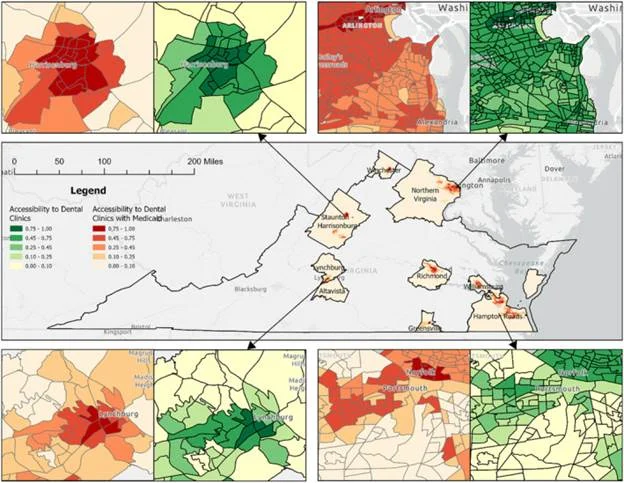
Figure: Transit-based dental access in Virginia shows major urban centers (Northern Virginia, Richmond, Hampton Roads) with high clinic availability (green) and rural towns (Greenville, Altavista) with very low accessibility (red).
Specific statistics on wisdom tooth care in Virginia are sparse, but general oral health data highlight rural–urban disparities.
A recent analysis of dental access in Virginia found that rural regions have far fewer reachable dental clinics: for example, residents of Greenville or Altavista have on average only ~1 or <1 dental clinic accessible by a 60-minute transit trip, whereas Northern Virginia residents have over 120 clinics within the same range.
Even fewer clinics accept Medicaid in those rural areas. These geographic barriers suggest rural Virginians may face long travel times for specialized care (like oral surgery) and lower rates of routine dental visits.
In practical terms, urban Virginians (e.g. Northern Virginia, Richmond) likely follow national extraction patterns, with easy access to oral surgeons and dental follow-up.
In contrast, rural Virginians may have delayed or less frequent extractions simply due to access issues, and may rely on general dentists for any surgical needs or travel long distances to specialists.
(Notably, Virginia’s Medicaid dental plan generally covers prophylactic third-molar removal only after consultant review, which could also influence when extractions are authorized.)
Overall, we infer that urban Virginia exhibits high procedure volumes similar to national trends, whereas rural areas may show lower extraction rates and possibly more conservative management by default.
Future Outlook and Forecasts

Looking ahead, several trends are emerging in wisdom tooth care. Demographically, as tooth preservation and caries prevention improve, more people may reach mid-adulthood with healthy asymptomatic wisdom teeth; this could modestly reduce the share of young people undergoing extraction.
In line with evidence-based shifts, active surveillance of asymptomatic third molars is likely to increase, reserving surgery for only those that show pathology or high future risk.
Technological advances will shape the future: for example, cone-beam CT imaging and possibly AI decision-support could better predict which wisdom teeth are likely to cause problems.
Surgical innovations like transoral robotic surgery (TORS) have been suggested as future tools to improve visibility and precision for difficult extractions.
Minimally invasive techniques (piezosurgery, endoscopy) and enhanced perioperative care (e.g. improved anesthesia, digital workflow) will continue reducing patient morbidity.
In terms of frequency, extraction rates may stabilize or decline slightly as guidelines tighten. Public health interest in value-based dentistry may further discourage unnecessary prophylactic extractions.
However, the sheer volume of teenagers entering wisdom-tooth-bearing age ensures that thousands of new extractions will still occur each year. Ultimately, forecasts emphasize a more personalized approach: combining better risk assessment tools with patient preferences and public health considerations.
Continued research (large-scale data studies, clinical trials) and updated state/national guidelines will guide providers on the optimal balance between removal and retention in the coming years.
Key Takeaways: Wisdom tooth surgery remains common in the U.S., with extraction rates highest in late teens/early 20s and regional variations by geography. Complication rates are relatively low (single-digit percentages), but given procedure volume they demand attention. In Virginia, urban areas have far better dental access than rural areas, likely influencing wisdom tooth care patterns. Future trends point toward more selective extraction practices, aided by technology and evidence-based guidelines.
References: Key data and statements are drawn from recent peer-reviewed studies and official sources. Notable references include national cohort analyses and systematic reviews, as well as Virginia Medicaid policy documents. The full list of sources is provided below.
- Schroeder AR, Newman TB, Girod S, Hashemi S, Häberle AD. Estimated cumulative incidence of wisdom tooth extractions in privately insured US patients. Front. Dent. Med. 2022;3:937165.
- Chen Y-W, Chi L-Y, Lee OK-S. Revisit incidence of complications after impacted mandibular third molar extraction: a nationwide population-based cohort study. PLoS One. 2021;16(2):e0246625.
- Cunha-Cruz J, McClellan L, Rothen M, Spiekerman C, Drangsholt M, Huang GJ. Recommendations for Third Molar Removal: A Practice-Based Cohort Study. Am J Public Health. 2014;104(4):735–743.
- Lee J, Feng B, Park JS, Foo M, Kruger E, Chaubal T. Incidence of lingual nerve damage following surgical extraction of mandibular third molars with lingual flap retraction: A systematic review and meta-analysis. PLoS One. 2023;18(2):e0282185.
- Pinto AC, Francisco H, Marques D, et al. Worldwide prevalence and demographic predictors of impacted third molars—systematic review with meta-analysis. J Clin Med. 2024;13(24):7533.
- Yamada S, Hasegawa T, Yoshimura N, et al. Prevalence of and risk factors for postoperative complications after lower third molar extraction: A multicenter prospective observational study in Japan. Medicine (Baltimore). 2022;101(32):e29989.
- Sifuentes-Cervantes JS, Carrillo-Morales F, Castro-Núñez J, Cunningham LL, Van Sickels JE. Third molar surgery: Past, present, and the future. Oral Surg Oral Med Oral Pathol Oral Radiol. 2021;132(5):523–531.
- Sarikov R, Šidlauskas A, Brilius A. Inferior alveolar nerve injury after mandibular third molar extraction: literature review. J Oral Maxillofac Res. 2014;5(4):e6.
- Kostares E, Kostare G, Kostares M, Tsakris A, Kantzanou M. Prevalence of surgical site infections following extraction of impacted mandibular third molars: A systematic review and meta-analysis. J Stomatol Oral Maxillofac Surg. 2025;126(1):101995.
- Cochrane Oral Health Group. Surgical removal versus retention for the management of asymptomatic disease-free impacted wisdom teeth. Cochrane Database Syst Rev. 2020;(5):CD003879.
- Virginia Department of Medical Assistance Services (DMAS). Cardinal Care Smiles Operating Requirements Manual. June 2025.