When you get a dental implant, the first three months after placement are the most critical period for long-term success.
Primary stability refers to the mechanical stability of your implant immediately after placement and plays a critical role in determining whether osseointegration will occur properly.
During these early weeks and months, dental implant stability for the first 90 days is critical because the implant must stay secure while new bone cells grow around it and form a lasting bond.
The success of your dental implant depends heavily on what happens during this initial healing period. Your implant needs to stay firmly in place while your body works to integrate it with the surrounding bone tissue. Too much movement during this time can disrupt the healing process and lead to implant failure.
Understanding what affects stability in these first 90 days can help you make better decisions about your treatment and recovery.
Research shows that multiple factors influence how well your implant stabilizes during this crucial window, including the implant design, your bone quality, and the surgical technique used by your dentist.
Modern assessment methods now allow dentists to monitor stability throughout the healing process. This article explains why these first three months matter so much and what you can do to give your implant the best chance of success.
Key Takeaways
- The first 90 days after implant placement are critical because your implant must achieve mechanical stability before bone integration can occur
- Primary stability depends on factors like implant design, bone quality, and surgical technique that your dentist can optimize
- Modern monitoring methods allow dentists to track your implant stability throughout healing to ensure successful osseointegration
The Importance of Implant Stability in the First 90 Days
Your dental implant needs two types of stability to succeed, and the balance between them shifts dramatically during the first three months after placement.
What Implant Stability Means
When dentists talk about implant stability, they’re describing how firmly your implant stays in place. There are two distinct types you need to understand.
Primary stability is the mechanical stability of the implant immediately after placement. Your dentist creates this by carefully fitting the implant into your jawbone. Think of it like screwing a bolt into wood—the threads grip the surrounding material right away.
Secondary stability develops over time through osseointegration. This is when your bone cells grow onto the implant surface and fuse with it. The process transforms your implant from a mechanical fixture into a biological part of your jaw.
During the first 90 days, primary stability gradually decreases while secondary stability increases. Your implant actually goes through a temporary dip in overall stability during this transition.
The Healing Timeline and Critical Window
Your bone begins remodeling around the implant within the first week. Studies show that a thin layer of new bone contacts the implant surface by day five.
The traditional healing timeline looks like this:
- Days 1-14: Initial wound healing and clot formation
- Weeks 2-6: Bone remodeling begins, primary stability decreases
- Weeks 6-12: New bone formation accelerates, secondary stability increases
- Week 12+: Mature bone integration completes
The critical window falls between weeks 2 and 8. During this period, your implant is most vulnerable because primary stability has weakened, but secondary stability hasn’t fully developed yet. According to a study, micromotion of less than 0.1 mm during this phase can trigger problems with bone healing.
Consequences of Instability in Early Healing
When your implant moves too much during the healing period, your body responds differently than intended. Instead of bone cells attaching to the implant surface, fibrous tissue forms around it. This soft tissue creates a barrier that prevents proper osseointegration.
The results are serious. Research shows that excessive stress around the bone-implant interface may induce fibrous tissue formation rather than direct bone contact, leading to implant failure. You might notice pain, swelling, or looseness if this happens.
Your success rate depends heavily on maintaining stability during these first months. Implants that achieve good primary stability and avoid excessive micromotion during healing show significantly higher long-term success rates.
That’s why your dentist gives you specific instructions about diet and activities after placement.
Biomechanics of Primary Stability
Primary stability depends on the mechanical friction between your implant and the surrounding bone at the moment of placement. The strength of this initial lock-in is determined by your bone characteristics, the physical design of the implant itself, and how tightly it’s secured during surgery.
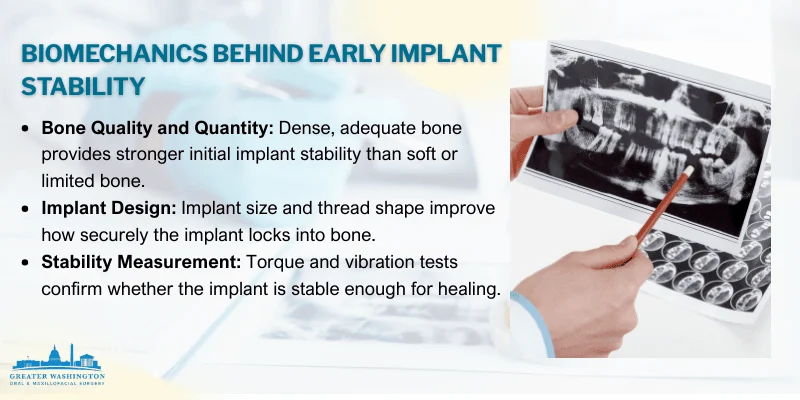
Bone Quality, Density, and Quantity
Your bone quality directly affects how well an implant can achieve initial mechanical stability. Dense cortical bone in your lower jaw provides better grip than the softer trabecular bone common in your upper jaw.
Bone density is measured in Hounsfield units (HU) on CBCT scans. Values above 850 HU indicate dense cortical bone that holds implants firmly. Values between 350-850 HU represent good quality bone, while anything below 350 HU suggests softer bone that may need modified placement techniques.
The thickness of your cortical bone matters most. Even a thin layer of dense cortical bone on the surface of your alveolar bone can provide sufficient friction to lock an implant in place. Your trabecular bone beneath contributes less to initial stability but becomes important during healing.
The amount of bone available also plays a role. Adequate height and width allow your dentist to place longer or wider implants that contact more bone surface area, creating stronger mechanical engagement.
The Role of Implant Design and Geometry
Your implant’s physical characteristics determine how effectively it engages with bone tissue. Thread design creates the mechanical lock that holds everything in place initially.
Key design features include:
- Thread geometry: Deeper threads with aggressive cutting edges grip bone more firmly
- Thread pitch: The spacing between threads affects how much bone is compressed during insertion
- Implant diameter: Wider implants contact more bone surface
- Implant length: Longer implants engage more cortical and trabecular bone
- Implant shape: Tapered designs compress bone as they’re placed, while cylindrical designs rely on precise drilling
Surface characteristics like roughness help but contribute more to long-term bone integration than immediate stability. Your implant macro-design and overall shape determine the initial mechanical engagement that matters most in the first few weeks.
The abutment connection doesn’t affect primary stability but becomes important once your implant starts bearing load.
Visit our Fredericksburg, Fairfax, Manassas, or Stafford clinics across VA to check your healing progress and protect your implant success.
Insertion Torque and Measurement Techniques
Insertion torque measures the rotational force needed to place your implant and indicates how tightly it’s locked into bone. Most dentists aim for values between 30-45 N·cm to ensure adequate stability for healing.
Higher torque values generally mean better primary stability. Your dentist can feel resistance during placement, but digital torque wrenches provide exact measurements. Values below 25 N·cm may require a longer healing period before loading.
Resonance frequency analysis (RFA) offers another way to assess stability. This technique measures vibrations in your implant and converts them to an implant stability quotient (ISQ). ISQ values range from 1-100, with scores above 60 indicating good stability.
RFA works by attaching a small device to your implant that creates vibrations. The way your implant vibrates reveals how firmly it’s held by surrounding bone. Unlike insertion torque, you can repeat ISQ measurements throughout healing to track progress.
Clinical Factors Impacting Stability in Early Months
Several clinical decisions you and your dentist make directly affect how stable your implant remains during the critical first three months. The drilling approach used during surgery, where the implant sits in your jaw, and your own health conditions all play major roles in determining success.
Surgical Technique and Drilling Protocols
The way your dentist prepares the bone site affects how firmly your implant holds. Drilling protocols and surgical technique are key factors in achieving good initial stability.
Under-drilling means making the hole slightly smaller than the implant width. This technique creates tighter contact between bone and implant. Your dentist may use this approach if you have softer bone that needs extra grip.
The osteotomy process involves creating the exact space for your implant. Speed, pressure, and cooling during drilling all matter. Too much heat can damage bone cells. Too little pressure might make the hole too loose.
Different drilling approaches include:
- Standard drilling for average bone density
- Under-prepared sites for softer bone areas
- Osseodensification to compact and strengthen bone
Your implant insertion torque measures how much force is needed to place the implant. Higher torque usually means better initial stability. Most successful implants need at least 35 Newton-centimeters of insertion force.
Implant Placement Location in the Jaw
Your implant location in the jaw dramatically changes stability outcomes. The mandible (lower jaw) typically offers better stability than the maxilla (upper jaw) because it has denser bone.
Front teeth areas in your lower jaw provide the best bone quality. Back teeth regions, especially in your upper jaw, often have softer bone. This softer bone may require delayed loading protocols instead of immediate loading.
Bone density varies by location:
- Lower front teeth: Hardest, densest bone (Type 1-2)
- Lower back teeth: Medium density bone (Type 2-3)
- Upper front teeth: Moderate density (Type 2-3)
- Upper back teeth: Softest bone (Type 3-4)
Immediate implant placement right after tooth extraction is convenient but more challenging. The socket might not provide complete stability. Your dentist may need bone grafting or ridge augmentation to fill gaps around the implant.
Patient-Related and Host Factors
Study shows that your personal health and habits significantly impact implant stability during early healing. Patient-related factors affect both immediate stability and long-term success.
Osteoporosis weakens your bone density throughout your body, including your jaw. If you have this condition, your dentist might choose bone augmentation techniques or avoid immediate or early loading protocols.
Smoking reduces blood flow to your healing tissues. This slows osseointegration and increases failure risk. Quitting before surgery improves your chances significantly.
Diabetes affects wound healing and infection resistance. Poor blood sugar control can delay bone formation around your implant. Well-managed diabetes allows for normal healing in most cases.
Your age matters less than your overall health. Older patients with healthy bones often do better than younger patients with poor bone quality or uncontrolled health conditions.
Modern Assessment Methods for Implant Stability
Dentists now use precise digital tools to measure how well your implant bonds with your jawbone. These measurements help your dental team decide when it’s safe to attach your permanent restoration.
Insertion Torque Value Analysis
Your dentist measures insertion torque values when placing your implant into your jawbone. This number tells them how much rotational force is needed to screw the implant into place. Higher insertion torque values usually mean better initial stability.
Most successful implants require at least 35 Ncm (Newton centimeters) of torque. Your dentist might aim for 45-50 Ncm if you’re getting immediate loading. The insertion torque measurement depends on your bone density and the implant design.
Your bone quality affects these readings significantly. Dense bone in your lower jaw typically gives higher values than softer bone in your upper jaw. But remember that insertion torque value only measures stability at placement. It can’t track how your bone heals around the implant later.
Resonance Frequency Analysis and ISQ
Resonance frequency analysis measures your implant stability at any time during healing. The device sends tiny vibrations through your implant and measures how it responds. You get a number called an ISQ (Implant Stability Quotient) score.
Your ISQ score ranges from 1 to 100. Scores above 70 indicate excellent stability. Scores between 60-69 show good stability, while anything below 60 means your implant needs more healing time.
The Osstell device is the most common tool for resonance frequency analysis. Your dentist can recheck your ISQ at different appointments without damaging anything. This helps them track your healing progress and decide the best time to load your implant.
The Periotest is another option that taps your implant and measures mobility. Lower values mean better stability.
Digital and Imaging Technologies
Cone beam computed tomography (CBCT) creates 3D images of your jawbone before and after implant placement. Your dentist uses these scans to check bone density, plan exact implant positioning, and monitor bone growth around your implant.
An intraoral scan captures digital impressions of your teeth and gums. This technology helps your dental team track tissue changes around your implant site. These scans are more comfortable than traditional impressions and give precise measurements.
CBCT imaging shows your dentist exactly how much bone surrounds your implant threads. They can spot any gaps or problems early. Some practices combine digital imaging technologies with computer software to predict your implant stability before surgery even begins.
Start your care with confidence by submitting the new patient form now, allowing us to understand your dental history, concerns, and goals before you arrive.
Implant Surface Engineering, Materials, and Long-Term Success
The physical characteristics of your implant’s surface and the materials used in its construction directly affect how well bone cells attach and grow during the critical first 90 days. Engineers have developed specific surface treatments and material innovations that speed up bone formation and improve stability.
Surface Treatments and Topography
The implant surface texture plays a major role in promoting bone cell attachment and growth. Manufacturers create different surface topographies through various treatments that change how your implant interacts with surrounding bone tissue.
Common surface treatment methods include:
- Sandblasting – Creates a rough surface that increases bone-to-implant contact
- Acid etching – Forms microscopic pits that help cells anchor to the implant
- Plasma spraying – Adds a coating layer that enhances bone integration
- Anodization – Builds an oxide layer that improves biocompatibility
Your titanium implant’s surface roughness affects how quickly bone cells migrate and multiply. Rougher surfaces typically provide more area for bone attachment compared to smooth surfaces.
Research highlights that surface modifications are critical for ensuring long-term success because they directly influence the healing response during those crucial first weeks.
Hydrophilic surfaces attract body fluids better than hydrophobic ones. This means blood and proteins coat the implant faster, which speeds up the bone formation process.
Material Innovations and Implant Types
Titanium remains the gold standard for dental implants because it forms a stable oxide layer that prevents corrosion and promotes bone integration. The most common titanium alloy, Ti6Al4V, offers excellent strength and fatigue resistance for long-term function.
Modern implant materials include:
| Material | Key Benefits | Considerations |
| Pure titanium | Excellent biocompatibility | Lower strength than alloys |
| Ti6Al4V alloy | High strength and durability | Potential ion release concerns |
| Zirconia | White color, metal-free | Risk of microcracking |
Your implant’s shape also matters for stability. Tapered implants mimic natural tooth roots and distribute forces better than older cylindrical designs. The tapered design requires less bone removal during placement and improves initial contact with surrounding bone.
Conical implants offer advantages in areas where bone quality is compromised. The shape of your endosseous implant affects how forces transfer from the implant crown through the implant threads into your jawbone.
Strategies to Enhance Bone-Implant Contact
Maximizing bone-to-implant contact (BIC) during the first 90 days determines whether your implant achieves solid integration. Researchers measure BIC through histomorphometry, which calculates the percentage of implant surface directly touching bone tissue.
Thread design significantly impacts your implant’s performance. Microthreads at the implant neck help preserve marginal bone by distributing stress more evenly. These tiny threads are especially important during the early healing phase when your bone is remodeling around the implant.
Key factors that improve bone-implant contact:
- Thread pitch – Closer spacing increases functional surface area
- Thread depth – Deeper threads enhance primary stability but may complicate insertion
- Face angle – Lower angles reduce shear forces on surrounding bone
Companies like Nobel Biocare engineer their implant threads to optimize force distribution at the bone-implant interface. The geometry of your implant material works together with surface treatments to create an environment where bone cells can attach, multiply, and form new tissue efficiently during those critical first three months.
Advances and Future Strategies to Maximize Early Stability
New technologies and surgical techniques are helping dentists predict and improve implant stability from the moment of placement. Digital tools allow for more precise planning, while advanced bone preparation methods enhance the initial bond between your implant and jaw.
Guided Surgery and Digital Planning

Digital planning tools now let your dentist see exactly where to place your implant before surgery even begins. Finite element analysis (FEA) uses computer models to predict how forces will affect your implant based on your bone density and implant design. This helps your surgeon choose the best implant size and angle for your specific jaw structure.
Guided surgery systems use 3D scans to create surgical guides that direct the drill to the exact planned position. This precision matters most in areas like the posterior maxilla, where bone is often softer and harder to work with. The guides help your dentist achieve better initial stiffness by positioning the implant optimally.
Some implants now feature buttress threads and other surface characteristics designed through FEA testing. These features distribute biting forces more evenly and increase removal torque values, which measure how firmly your implant sits in the bone. Devices like Osstell can measure stability using resonance frequency analysis, giving your dentist real-time feedback during placement.
Adjunctive Techniques and Bone Remodeling Support
Osseodensification represents a major shift in how dentists prepare your jaw for implants. Instead of cutting bone away with traditional drills or osteotomes, this technique uses special burs that compress and expand bone outward. This increases bone quantity around the implant threads and improves initial contact.
The compressed bone acts as a denser foundation during early bone remodeling, when your body is actively rebuilding around the implant. This technique works especially well when your bone density is low or when immediate loading is planned.
Bone augmentation procedures can build up areas where bone volume is insufficient. Your dentist might add grafting materials during or before implant placement to support stability throughout the critical first 90 days.
Concerned About Implant Healing? Begin your dental care journey today with our team of experts and ensure your implant is integrating properly.
Frequently Asked Questions
The first three months after implant placement involve careful attention to stability measures, healing indicators, and daily habits that support bone integration. Understanding torque values, recognizing normal healing signs, and avoiding certain behaviors can make the difference between success and complications.
What are the critical factors for dental implant success in the first three months?
Your implant’s success depends heavily on achieving adequate primary stability at placement. Primary stability is the mechanical stability of the implant right after surgery and plays a critical role in long-term success.
The insertion torque value matters significantly during this period. Most studies use torque values between 30 and 45 N cm as the immediate loading threshold to ensure your implant stays stable during bone integration.
Your bone quality and quantity directly affect how well your implant locks into place. Dense bone provides better mechanical grip than soft bone, which is why your dentist evaluates your bone structure before surgery.
The surgical technique your dentist uses impacts your initial stability too. Proper drilling speed, depth, and width create the ideal fit between your implant and bone.
Can you explain how initial stability impacts long-term outcomes for dental implants?
Initial stability allows your implant to bridge the critical gap until secondary stability takes over through bone growth. Without adequate primary stability, your implant may experience micromotion exceeding 0.1 mm during early healing.
Excessive micromotion can trigger fibrous tissue formation instead of direct bone contact. This fibrous tissue prevents proper bone integration and leads to implant failure.
Your implant needs to remain mechanically stable for 3 to 4 months in the lower jaw and 6 to 8 months in the upper jaw. During this time, your body replaces damaged bone around the implant with new, healthy bone.
Studies show that thin layers of new bone begin contacting the implant surface around day five after placement. By three months, newly formed bone containing healthy bone cells replaces the original bone area around your implant.
For dental implant care, what are the best practices during the early healing period?
You need to avoid putting pressure on your implant during the initial healing phase. Hard or chewy foods can create forces that disrupt the bone integration process.
Keep the surgical site clean through gentle brushing and rinsing with prescribed mouthwash. Proper oral hygiene prevents infection without disturbing the healing tissue.
Take all prescribed medications exactly as directed by your dentist. Antibiotics and anti-inflammatory medications help control infection and reduce swelling.
Attend all follow-up appointments so your dentist can monitor your healing progress. These visits allow early detection of any potential problems.
Avoid smoking completely during the first 90 days. Smoking restricts blood flow to the surgical site and significantly increases your risk of implant failure.
What signs should I look for to know if my dental implant is healing properly?
Normal healing includes mild swelling and discomfort that gradually decreases over the first week. Your pain should be manageable with prescribed pain medication.
The surgical site should not show excessive redness, heat, or discharge. A small amount of clear or light pink fluid is normal, but thick yellow or green discharge signals infection.
Your implant should feel firmly in place without any movement or looseness. Any mobility you can feel with your tongue or finger indicates a stability problem.
Numbness in your lower lip that persists beyond a few days may indicate nerve involvement. Contact your dentist immediately if you experience ongoing numbness.
You should not have persistent bad taste or smell coming from the implant area. These symptoms often indicate bacterial infection requiring treatment.
How do lifestyle choices affect the stability and integration of my new dental implant?
Your smoking habit poses the biggest threat to implant success during the first 90 days. Nicotine constricts blood vessels and reduces oxygen delivery to healing bone tissue.
Poor nutrition slows your bone healing and weakens the integration process. You need adequate protein, calcium, and vitamin D to support new bone formation around your implant.
Excessive alcohol consumption interferes with bone healing and increases infection risk. Limit or avoid alcohol during the critical first three months.
Physical activities that risk facial trauma should be avoided until your implant fully integrates. Contact sports or activities with fall risks can damage your healing implant.
Stress and poor sleep affect your immune system and slow healing. Getting adequate rest helps your body focus energy on bone integration.
What are the potential risks during the first 90 days after getting a dental implant and how can they be minimized?
Infection ranks among the most common early complications you might face. You can minimize this risk by maintaining excellent oral hygiene and taking prescribed antibiotics.
Implant failure due to inadequate stability happens when your bone quality is poor or surgical technique is compromised. Your dentist can reduce this risk by properly assessing primary stability through insertion torque and resonance frequency analysis.
Nerve damage can occur if your implant is placed too close to nerve structures. Your dentist uses imaging, such as CT scans, to plan safe implant placement away from nerves.
Excessive force from chewing can cause micromotion and prevent proper bone integration. You protect your implant by following dietary restrictions and avoiding hard foods.
Sinus complications may develop if upper jaw implants penetrate the sinus cavity. Proper surgical planning and technique prevent this issue from occurring.




